Biological Dentistry in NYC and East Hampton
A non-toxic approach to oral wellness
The link between the mouth, body, mind, and spirit holds the key to optimal health and longevity
Our approach to wellness starts with the mouth. Realizing the link between the mouth, body, mind, and spirit holds the key to optimal health and longevity. Unlike conventional dentistry, which is mostly geared towards treating symptoms, biological dentistry looks at the whole person to evaluate health and wellness needs. This includes the complete spectrum of a patient’s biology, from their gut biome and their oral and physical health to their emotional and even spiritual well-being. The goal of biological dentistry is not only to resolve symptomatic issues, but to get to the root of what’s causing symptoms in the first place.
Explore our biologic dental services
THE NON-TOXIC, HOLISTIC APPORACH TO ORAL HEALTH
ABOUT BIOLOGICAL DENTISTRY
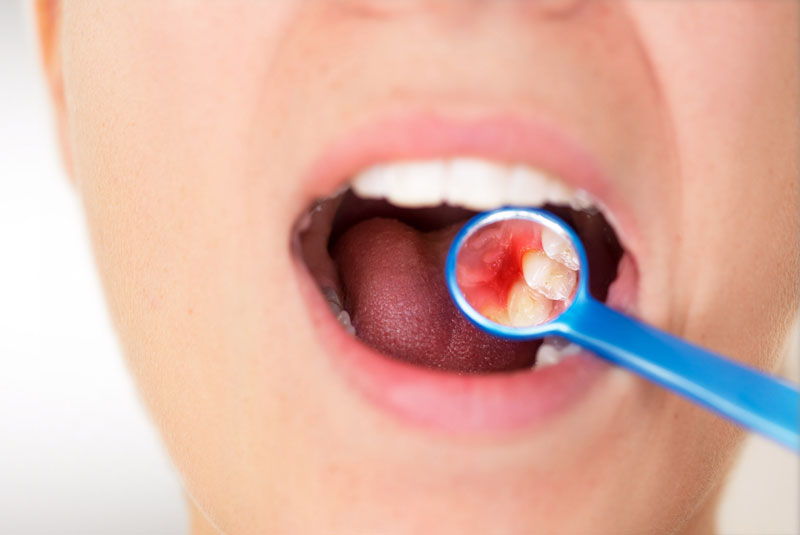
The mouth is so often overlooked, but it actually is the gateway and a mirror to your entire body.You can’t be truly well without a healthy mouth.
“A Healthy Body Begins with a Healthy Mouth. Your oral health is a crucial cornerstone for disease prevention, longevity, and a vibrant life.”
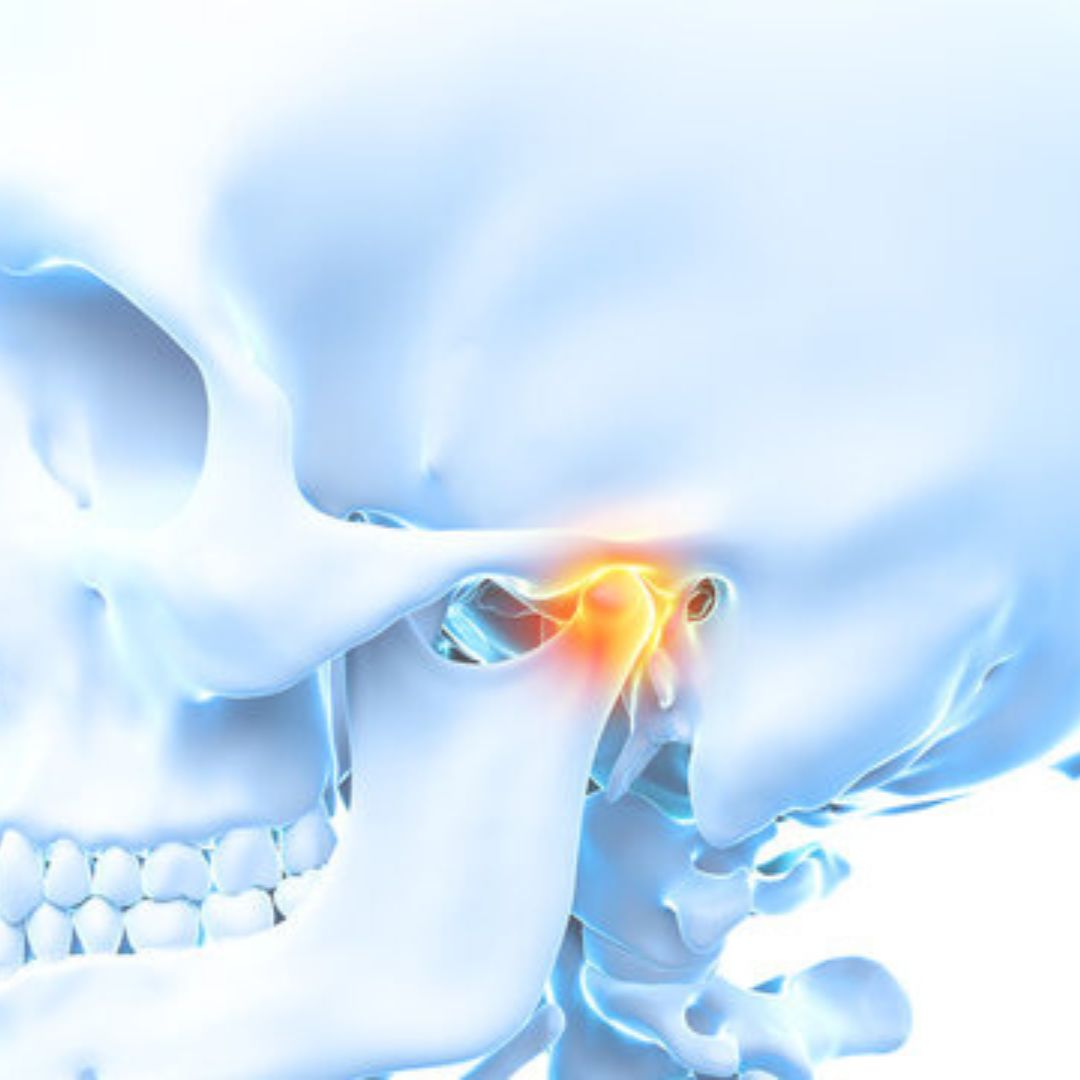
TMJ can cause more than just jaw pain
Dr. Gerry Curatola employs cutting-edge technology to comprehensively assess every facet of a patient’s well-being, encompassing genetics, metabolism, biochemistry, and emotional behavior. By doing so, the Rejuvenation Health team can pinpoint the underlying causes of diseases and enable the body to rejuvenate its innate self-healing capabilities. Extensive research confirms the profound connection between oral health and disease prevention. The primary objective of our team of biological dentistry experts is to eliminate toxins, facilitating the body’s innate healing and repair mechanisms in the most efficient, effective, and natural manner possible. more
At Rejuvenation Health, everything we do is with a biologic lens. A focus on overall oral health and the body’s natural biological processes always comes first, and our goal is to enhance the appearance of a patient’s smile while also taking into account the long-term health and well-being of the teeth and surrounding oral structures. The Rejuvenation approach recognizes the interplay between aesthetics and biology in dentistry.
Meet Your Biologic Dental Team





Meet with us virtually schedule your consult with Dr. Curatola and team
Step One: Comprehensive in person or telehealth consultation with Rejuvenation Health Team
Step Two: Customized treatment plan development and review
Step Three:Treatment scheduling with a dedicated patient coordinator
Step Two: Customized treatment plan development and review
Step Three:Treatment scheduling with a dedicated patient coordinator
Teeth whitening
Many people desire white teeth and a straight smile, but the methods chosen matter. Home whitening kits are accessible, but improper use may lead to future problems. Professional teeth whitening is a safer and more effective choice. It offers immediate results and expert guidance, ensuring your oral health remains protected.
TMJ therapy
Suffering from facial muscle soreness or jaw pain? The Rejuvenation Health team, led by Dr. Curatola, a pioneer in biological dentistry, is here to ease your discomfort. We specialize in holistic treatments to relieve chronic pain and improve your overall well-being, especially when vague symptoms affect your daily life, like eating and sleep quality.
Rejuvenation Mouth Facial™
The Rejuvenation Mouth Facial is a novel approach to oral health inspired by skin facials. It begins with a comforting Himalayan salt “sole” rinse, followed by a gentle tooth scaling to eliminate plaque, tartar, and stains. We then apply Dr. Curatola’s exclusive antioxidant “gum mask” featuring NuPath Bioactives®, a combination of vitamins, mineral salts, prebiotics, and herbal ingredients, to rejuvenate and nourish your teeth and gums.
Proactive preventive dentistry
Regular dental checkups and cleanings are essential for a healthy smile and overall well-being. Combining good at-home care with visits to a biological dentist is crucial for maintaining healthy teeth and gums. Proactive dentistry also contributes to overall wellness by preventing and treating systemic illnesses like heart disease, cancer, and pregnancy complications. Our dedicated team of specialists takes a holistic approach to your dental care, aligning it with your overall health.
A highly personalized, holistic treatment experience to unlock the life-force within.
